Coping with autism can feel like a sudden shift in gravity. Relief and grief, clarity and confusion, all crowd in at once. There is the label (with that comes the stigma), the paperwork, and the inevitable questions.
And then the quiet pause of “Now what?”
Long before that moment, though, many live through a drawn-out pre-diagnosis phase. Includes studying, noting patterns, and preparing questions for the consultant. These steps, modest as they seem, help steady the ground and make the conversation ahead more coherent.
Our guide on coping with autism diagnosis is meant as a compass through both stages—the groundwork before diagnosis and the path that unfolds after. Up next, we’ll break down what the diagnosis truly means and how to cope with autism in daily life.
Read on.
Coping with Autism Diagnosis: What It Means

You’ve heard the word. You’ve sat through the explanation.
Now you’re holding a diagnosis that’s supposed to help, but doesn’t quite tell you how. Even with a name, coping with autism spectrum disorder is rarely straightforward – it often opens a new set of questions you didn’t know you’d be asking.
Pam Aculey, parent of a child on the spectrum, says, “Receiving our son’s autism diagnosis was a life-changing moment. Whilst it provided us with an explanation… it also instilled panic, confusion and uncertainty for the road ahead.”
That mix of clarity and overwhelm is something many families feel in the days that follow. Understanding the different diagnostic labels is the first step in finding autism coping skills that actually fit.
Your child meets the criteria for Autism Spectrum Disorder, Level 2

This statement reflects the current diagnostic model under the DSM-5, where autism is recognized as a spectrum rather than distinct subtypes like Asperger’s or PDD-NOS.
Level 2 suggests substantial support needs, especially in areas like social interaction, communication, behavioral flexibility, and sensory regulation.
You may notice:
- Frequent meltdowns when routines change
- Limited back-and-forth interaction
- Delayed speech or unusual language patterns
- High sensitivity to noise, touch, or crowds
What this might mean:
- Referrals for speech therapy, occupational therapy, and behavior-based interventions
- Likely need for a special educator or shadow teacher in inclusive settings
- Monthly therapy expenses in private setups can run ₹15,000–₹30,000+
- Eligible for disability certification under the RPwD Act, which can support access to schools, concessions, and future government schemes
Often, children at this level may also be evaluated for co-occurring conditions like ADHD, sensory processing difficulties, or speech apraxia. Each of these can shape therapy goals and timelines. Families often ask how to cope with autism when support needs are substantial. At this level, coping strategies for autism usually include speech therapy, occupational therapy, structured routines, and professional guidance.
Traits consistent with autism, Level 1

Level 1 autism indicates milder but still impactful support needs. Individuals may have fluent language and average cognitive abilities, but experience difficulty with social nuance, rigidity, anxiety, or sensory overload. These are often internal struggles that others don’t easily see.
This is where high functioning autism coping strategies often come into play – building social confidence, coaching for executive skills, and offering tailored counseling.
What this might mean:
- May go unnoticed in school unless academic or emotional challenges appear
- Needs may include counseling, executive function coaching, or group therapy
- Girls and verbally articulate children may mask symptoms, leading to delayed or missed diagnosis
- Support may feel optional to others, but burnout and withdrawal are real risks
- Financially, it often means unstructured, ongoing out-of-pocket expenses for private support with little formal recognition
Diagnosis at this level may be made later in life, especially in women, nonbinary individuals, or those misdiagnosed with anxiety, OCD, or depression. For adults, it can feel like both clarity and reckoning.
ADHD and autistic features are both present

This is a dual diagnosis that’s becoming more widely recognized. ADHD and autism often overlap, with each condition amplifying the other’s challenges. A child might struggle to sit still and also resist transitions. An adult might be impulsive, yet hyper-focused and anxious in new social situations.
What this might mean:
- Need for a combined intervention plan: behavioral therapy, sensory tools, and classroom strategies
- In some cases, medication may be advised to manage inattention or hyperactivity
- School systems may struggle to support both diagnoses simultaneously
- Costs can quickly add up—between therapy, psychiatric consults, and parental guidance
- Most insurance plans don’t fully cover these needs in India
Clinicians often highlight this combination to explain why a child doesn’t respond to a single therapy style—or why social skills improve, but regulation doesn’t.
Parents may need to explore combined coping mechanisms for autism and ADHD, including behavioral therapy and school accommodations.

Social Pragmatic Communication Disorder fits better
This diagnosis is given when social interaction is affected—like difficulty understanding tone, taking turns in conversation, or interpreting gestures—but without the repetitive behaviors or sensory differences seen in autism.
It’s considered distinct from ASD, but support is still essential. What this might mean:
- May be referred to speech-language therapy focused on social communication
- Often excluded from autism-specific school accommodations and benefits
- Teachers may misread challenges as immaturity or rudeness
Parents sometimes ask how they’re supposed to hold it all together. The answer isn’t about perfection so much as steadiness.
![]()
Your own regulation is the anchor. If you can stay steady, you’ll catch the small signs of frustration and step in before it tips into a breakdown. Every problem cannot be immediately fixed but just staying watchful will help you detect if your child is getting pushed over the edge, and you can check that in time!
Puja Dutta, RCI-registered Clinical Psychologist at India Autism Center
Long-term support is still needed, but legal protections and public funding are limited. This diagnosis can feel ambiguous for parents, but the key is not waiting. Social communication skills can improve dramatically with early, targeted support.
Even without a full autism diagnosis, families benefit from autism coping skills for adults and children alike – skills like emotional regulation, communication strategies, and sensory support.

Developmental delay with autistic features; we’ll reassess
Used for children under 5 when delays are observed across areas—like speech, motor skills, or play—but a full autism diagnosis is not yet confirmed. It’s a watch-and-intervene approach.
This overlaps with Global Developmental Delay (GDD), a term that gives space to monitor evolving needs.
What this might mean:
- Begin early intervention immediately: speech, OT, special education
- Track milestones closely, with reassessments every 6–12 months
- May receive temporary disability certification to access early support
- Therapy costs are often high upfront, with limited public provision
- Diagnosis may later evolve into ASD, ID, or a learning disability, depending on the child’s developmental path
Early intervention here focuses less on labels and more on developing autism coping skills – speech, play-based learning, and structured support routines.
So, now that you’ve unpacked the language, let’s move toward what to actually do with it. Next up: building a plan, finding the right support, and making this diagnosis work for you.

Personalizing Support: What to Focus on, What to Let Go
Parents of autistic children are often handed a flood of advice. New therapies, new strategies, new “essentials.” What gets lost in that rush is a quieter truth: not every approach matters equally. What matters most is finding coping strategies for autism that fit the child in front of you.
Support becomes clearer when you slow down long enough to notice. Which moments seem to calm? Which spark tension? Which gestures or sounds carry meaning? A pattern begins to reveal itself, and with it, the outline of a plan.
Seen this way, the next steps become clear.
Decode Sensory Clues Before Labeling Behavior
A child covering their ears in a crowded room is not being difficult; they are signaling distress. A refusal to wear a certain shirt may point less to stubbornness than to the irritation of a seam. Behavior, in this sense, is language—sometimes subtle, often urgent.
Check these common sensory signals found in autism and ways to respond:
| If You Notice This | It May Reflect | You Can Try |
| Hands clamped over ears | Auditory sensitivity | Noise-canceling headphones, quiet breaks |
| Refusal of clothes/shoes | Tactile discomfort | Softer fabrics, tagless clothing |
| Chewing on sleeves or pencils | Oral sensory-seeking | Chewelry, crunchy snacks |
| Pacing, spinning, or jumping | Need for movement | Swings, trampolines, and climbing breaks |
| Withdrawal in bright rooms | Visual overload | Dim lighting, sunglasses |
When interpreted this way, behavior shifts from being a problem to be managed to a clue about how the world is being experienced.
This forms part of everyday coping mechanisms for autism, helping children regulate without escalating stress.
Use Routine to Create Safety, Not Rigidity
Routines are often described as restrictive, but for many autistic children, they serve as anchors. Predictability eases anxiety, creates a sense of safety, and makes daily life less chaotic. The goal is not rigid adherence to schedules but a rhythm steady enough to provide reassurance.
Ways routines can ease daily life:
| Goal | Tool That Helps |
| Calmer mornings | Picture strip by the mirror |
| Smoother bedtimes | Dimmer switch + checklist |
| Easier transitions | Countdown timer + verbal cue |
| Less chaotic weekends | “Today’s Plan” fridge chart |
Sometimes the most effective support is not a full overhaul but a small, consistent addition that lowers stress.
For many families learning how to live with autism, routines become a key autism coping skill that provides both safety and flexibility.
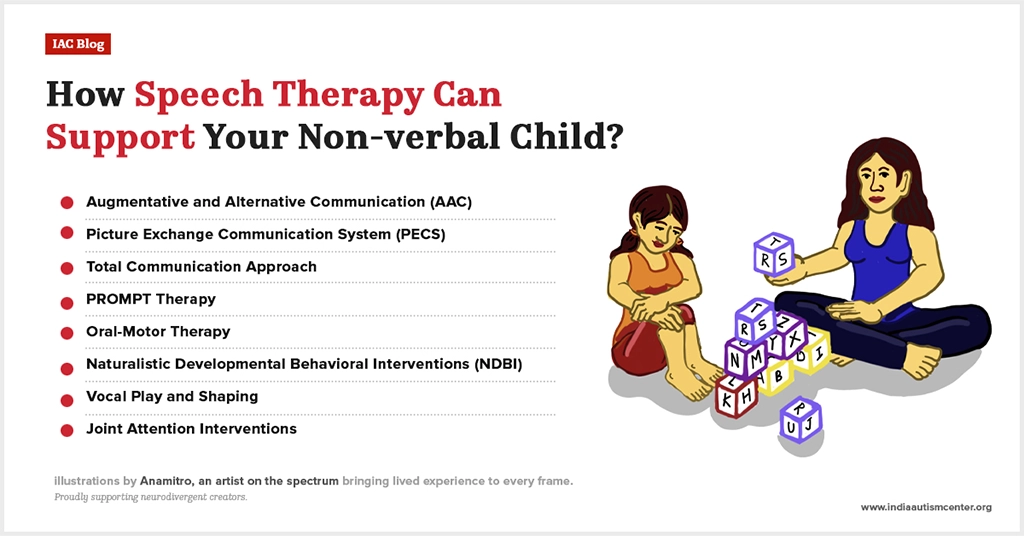
Expand Communication Beyond Speech
Spoken words often arrive unevenly, or not at all. Yet communication rarely disappears. It shows up in gestures, repeated phrases, the rhythm of movement, or with the help of assistive devices. To recognize those signals is to widen the frame of what language looks like.
Ways to make communication more accessible:
- Offer clear picture choices instead of open-ended questions
- Treat repeated scripts as openings, not interruptions
- Allow extra pauses before stepping in
- Keep AAC tools close during everyday routines
By shifting attention from what is absent to what is present, communication begins to feel broader, more possible.
Communication supports are essential coping skills for autism spectrum disorder, especially when speech is delayed or absent.
Teach Regulation Before the Storm
Meltdowns rarely arrive without warning. They build gradually—restlessness, escalating scripts, withdrawal. These are not minor inconveniences but early signals that the child is nearing a breaking point. Intervening before escalation often means the difference between a spiral and a moment of calm.
Here are some early clues and supports that prove useful:
| Early Clue | Helpful Support |
| Pacing or restless hands | Fidget tools, deep pressure |
| Escalating scripts | Calm break, quiet corner |
| Covering ears or eyes | Headphones, dim lights |
| Repeated questions | Visual schedule, consistent reply |
Calm practices introduced early and often, not in the midst of a crisis, are the ones most likely to take hold. These proactive methods are some of the most reliable autism coping skills for adults and children.
Start With Strengths, Not Deficits
The impulse to focus on delays is strong, but strengths are often the more reliable path forward. A child’s fascinations, talents, or even quirks can become tools for learning and connection. What lights them up can also guide them toward growth.
Transform strengths into supports:
| Strength | How to Build On It |
| Fascination with trains | Counting, turn-taking, sequencing |
| Love of drawing | Self-made visual schedules |
| Strong memory for patterns | Anchoring routines and rules |
| Mimicry of sounds | Social scripts and play |
| Passion for animals | Responsibility and empathy-building |
When growth is anchored in strength, progress often feels less like correction and more like expansion. This strength-based model not only builds skills but also teaches coping strategies for autism by creating positive learning anchors.
Support, then, is not about adding more. It is about finding the shape that matches a child’s needs and leaning into it. Observed closely, the outline is already there.
Use Cognitive Training to Strengthen Core Skills
In India, cognitive training is slowly gaining traction as an essential part of intervention for children with developmental differences. Unlike therapies that target specific behaviors, cognitive training strengthens the “thinking skills” beneath them with flexibility, self-regulation, multitasking, working memory, and problem-solving. These are the foundations that help a child adapt in the classroom, manage frustration, and carry new learning into daily life.
Why it matters: Without these skills, even strong abilities, like language or memory, may not translate into independence. A child who can memorize facts may still struggle to shift when plans change; one who speaks fluently may still be derailed by poor regulation. Cognitive training fills these gaps by teaching children how to manage information, not just absorb it.
For many, especially when coping with ASD as an adult, cognitive training becomes a crucial tool for independence and daily functioning.
What it looks like:
- Memory and sequencing games to strengthen working memory
- Structured play that encourages flexible thinking
- Daily activities that demand planning and self-monitoring
Looking Ahead: Financial Foundations for Lifelong Support

Financial planning becomes essential once an autism diagnosis enters a family’s life. It is the start of a long journey to ensure your child’s needs are met today and protected for tomorrow. A strong financial plan is just as vital as therapies and coping skills for autism. It ensures that support systems continue long-term, especially as children transition into adulthood.
In India, families can explore government-supported Niramaya Health Insurance, covering hospitalization and therapy, or private options like Star Special Care, which includes medical, therapy, and hospital expenses. Internationally, programs such as UnitedHealthcare Special Needs Plans or AXA disability coverage offer comprehensive long-term support. These plans do more than pay bills. They create a safety net that lets daily life unfold with less uncertainty.
A thoughtful financial strategy brings calm and confidence. Planning early safeguards not just care, but your child’s dignity and future possibilities. If you’re unsure which options fit best, a consultation with a specialist can help map the path forward.
Frequently Asked Questions
Coping skills are strategies that help manage sensory sensitivities, emotional regulation, and social interactions. They can include routines, mindfulness exercises, sensory tools, and structured problem-solving approaches.
Autistic individuals use a mix of self-developed routines, environmental adjustments, and support networks. Some rely on structured schedules, hobbies, or technology, while others use therapy-informed strategies to navigate social or sensory challenges.
Yes – autism does not preclude a fulfilling, independent life. “Normal” is relative, but with support, skills development, and accommodations, autistic people pursue education, careers, relationships, and hobbies like anyone else.
Adult coping often focuses on self-advocacy, emotional regulation, and building sustainable routines. Leveraging therapy, peer support, workplace accommodations, and personal strengths helps navigate daily demands and life transitions effectively.
Coping with autism as a parent involves balancing emotional support, structured routines, and consistent therapy for your child. Understanding your child’s sensory cues, building communication strategies, and seeking support networks can make daily life smoother.
Effective coping strategies include maintaining predictable routines, using visual schedules, leveraging cognitive training, and focusing on your child’s strengths. Behavioral therapy, speech and occupational therapy, and family counseling also play a vital role. For more personalized coping strategies for autism, you can reach out to the experts at IAC. Contact us for guidance.
Nonverbal children can often communicate through gestures, picture cards, AAC tools, or repetitive scripts. Recognizing these signals as language and encouraging alternative communication methods is essential.
Resources include early intervention centers, speech and occupational therapy services, special educators, and government programs like disability certification under the RPwD Act. Private insurance options like Niramaya Health Insurance or Star Special Care can help manage therapy costs. For a personalized roadmap to these resources, reach out to IAC.
Yes! Adults on the autism spectrum can develop coping skills through cognitive training, social skills coaching, and structured routines. Learning self-regulation, mindfulness, and stress management strategies can significantly improve quality of life.