When a person is diagnosed with a disability, whether it is autism or another disability, the journey ahead often involves therapy, assistive devices, education support, and long-term care planning.
The challenge is not just emotional but also financial and logistical. This is where structured government initiatives like the Deendayal Disabled Rehabilitation Scheme DDRS come into play. The initiative can be a game-changer as India has over 2.68 crore persons with disabilities as per the Census of 2011.
Moreover, a large chunk of this number still lacks access to structured rehabilitation services. Schemes like the DDRS thus aim to bridge this huge gap by strengthening grassroots rehabilitation services as well as empowering organisations to deliver support where it is needed most.
If you are a parent of a child with autism, a caregiver, or part of an NGO, this guide helps you understand how the Deendayal Disabled Rehabilitation Scheme can help you unlock real, tangible support.
What is the Deendayal Disabled Rehabilitation Scheme?

The Deendayal Disabled Rehabilitation Scheme (DDRS) is an initiative by the Government of India. It is designed to support voluntary organisations that provide rehabilitation services to persons with disabilities.
In essence, the government does not directly run the services; it funds NGOs and rehabilitation institutions so they can offer important services such as therapy, education, vocational training and community-based rehabilitation.
Key Objective of DDRS:
The primary goal of the DDRS scheme is to:
- Create accessible rehabilitation services across India
- Strengthen institutional and community-based rehabilitation models
- Support persons with disabilities in achieving independence
- Promote inclusion in education, employment, and society
For families dealing with autism, this means access to therapy centres, early intervention programs, and structured support systems.
The Vision and Objectives of the DDRS Scheme

The core objective of the DDRS scheme is to ensure the correct implementation of the Rights of Persons with Disabilities Act, 2016. It focuses on several key areas such as:
1. Ensuring Equal Opportunities: By funding special schools and centres, the DDRS ensures that children with neurodivergent conditions have the same learning opportunities as their peers.
2. Empowerment through Inclusion: The rehabilitation assistance scheme helps through the transition from specialised environments to inclusive community living.
3. Resource Optimisation: It utilises the infrastructure of a district disability rehabilitation centre to provide technical support and equipment to those in need.
4. Social Justice: It aims to protect the rights of the disabled by making rehabilitation services affordable or free for the underprivileged.
Why DDRS Matters for Autism and Developmental Disabilities?

Autism requires long-term, consistent support. This includes therapies like speech therapy, occupational therapy, behavioural interventions, and structured education.
Here is why the rehabilitation assistance scheme under DDRS becomes important:
- Early intervention can significantly improve developmental outcomes.
- According to global studies, early therapy can improve communication and adaptive behaviour in children who have autism.
- However, access to trained professionals remains limited in many parts of India.
- DDRS-supported centres help bring these services closer to communities.
Types of Projects Supported Under DDRS

The DDRS scheme is designed to support a wide range of rehabilitation services so that persons with disabilities, including autism, can receive care at different stages of life. Instead of focusing on just one type of support, the Deendayal Disabled Rehabilitation Scheme funds multiple project models through NGOs and institutions
This ensures that families can access early intervention and education, therapy, and livelihood opportunities under one broader ecosystem.
Special Schools
Special schools supported under the DDRS provide structured education for children with disabilities who may not be able to cope in mainstream classrooms without support. These schools focus on individualised learning plans, therapy integration, and skill-building activities.
For children with autism, this often includes communication training, behaviour support, or social skills development as per the requirement. Many of these schools tend to work closely with parents so that learning can be continued at home.
District Disability Rehabilitation Centres
The district disability rehabilitation centre model focuses on decentralising services so that families in rural and semi-urban areas can get complete access to necessary support without travelling long distances.
These centres provide basic therapy, assistive devices, awareness programs, as well as referrals to higher-level care when needed. They play a key role in bridging the urban-rural gap in disability services.
Early Intervention Centres
Early intervention is one of the most critical components of the rehabilitation assistance scheme. These centres cater to children usually below the age of six, where developmental delays can be identified and addressed early.
Services include speech therapy, occupational therapy, sensory integration, and even parent training. Research consistently shows that early support is significantly helpful in improving long-term outcomes in children with autism, making these centres a cornerstone of the Deendayal Disabled Rehabilitation Scheme DDRS.
Residential and Community-Based Rehabilitation Projects
The Deendayal Disabled Rehabilitation Scheme offers support for residential care facilities and community-based rehabilitation programs. Residential facilities aim to offer long-term care for persons who are in need of constant supervision, while community-based programs focus on integrating persons with disabilities into society.
These initiatives emphasise life skills, social participation, and dignity, which are necessary for holistic rehabilitation.
Vocational Training Centres
For older children, adolescents, and adults, vocational training centres funded under the DDRS scheme help build independence. These centres offer skill-based training such as tailoring, computer skills, handicrafts, and other income-generating activities.
For individuals who are diagnosed with autism, structured vocational environments can improve focus, routine-building, and confidence, ultimately supporting long-term employment or self-employment.
Who Can Benefit from DDRS?
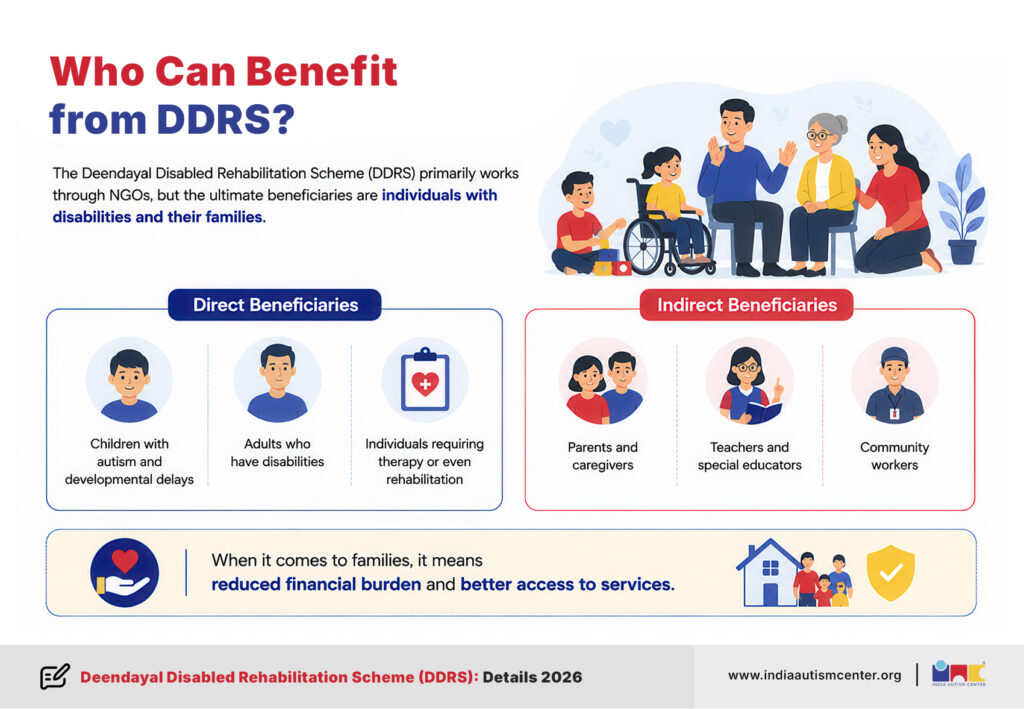
The Deendayal Disabled Rehabilitation Scheme DDRS primarily works through NGOs, but the ultimate beneficiaries are individuals with disabilities and their families.
Direct beneficiaries include:
- Children with autism and developmental delays
- Adults who have disabilities
- Individuals requiring therapy or even rehabilitation
Indirect beneficiaries:
- Parents and caregivers
- Teachers and special educators
- Community workers
When it comes to families, it means reduced financial burden and better access to services.
What is the Eligibility Criteria for Organisations?

The DDRS scheme gives funding to eligible NGOs and institutions. To qualify, organisations need to:
- Be legally registered
- Have at least two years of experience in disability services
- Possess basic infrastructure and trained staff
- Maintain transparency in financial records
How to Access DDRS Services as a Parent?

Getting started with the DDRS scheme is quite manageable when you break it into clear steps. Since the Deendayal Disabled Rehabilitation Scheme operates through NGOs and local centres, your focus should be on finding the right support system near you and staying actively involved.
Here are the steps that you can follow:
Step 1: Look for NGOs or a district disability rehabilitation centre through your district social welfare office, hospitals, or trusted disability networks.
Step 2: Speak to staff to understand what services are available under the rehabilitation assistance scheme, such as therapy, special education, or skill training.
Step 3: Keep your child’s disability certificate, medical records, and ID proof ready during the registration process
Step 4: Most centres will evaluate your child’s needs before recommending suitable programs
Step 5: Choose programs that match developmental requirements for your child
Step 6: Attend parent training sessions. Also, make sure to follow therapy practices at home to maximise the benefits of the DDRS.
What are the Challenges During Implementation of the DDRS Scheme?

While the Deendayal Disabled Rehabilitation Scheme DDRS has created a meaningful impact, its effectiveness is often limited by on-ground challenges. These gaps can affect how families access services under the DDRS scheme, especially in smaller towns and rural areas.
Here are some of the most common issues:
- Limited awareness among families: Many parents are still unaware of the DDRS scheme, which means eligible children miss out on early intervention and therapy support
- Uneven distribution of centres: Services are often concentrated in urban areas, while several districts lack properly functioning district disability rehabilitation centre facilities
- Delays in fund disbursement: NGOs sometimes face delays in receiving funds, which tend to disrupt services and reduce program efficiency
- Shortage of trained professionals: There is a significant gap in qualified therapists, special educators, and rehabilitation experts across India
Because of these challenges, the reach of the DDRS remains uneven, making awareness and stronger implementation critical for better outcomes.
Tips for Parents and Caregivers
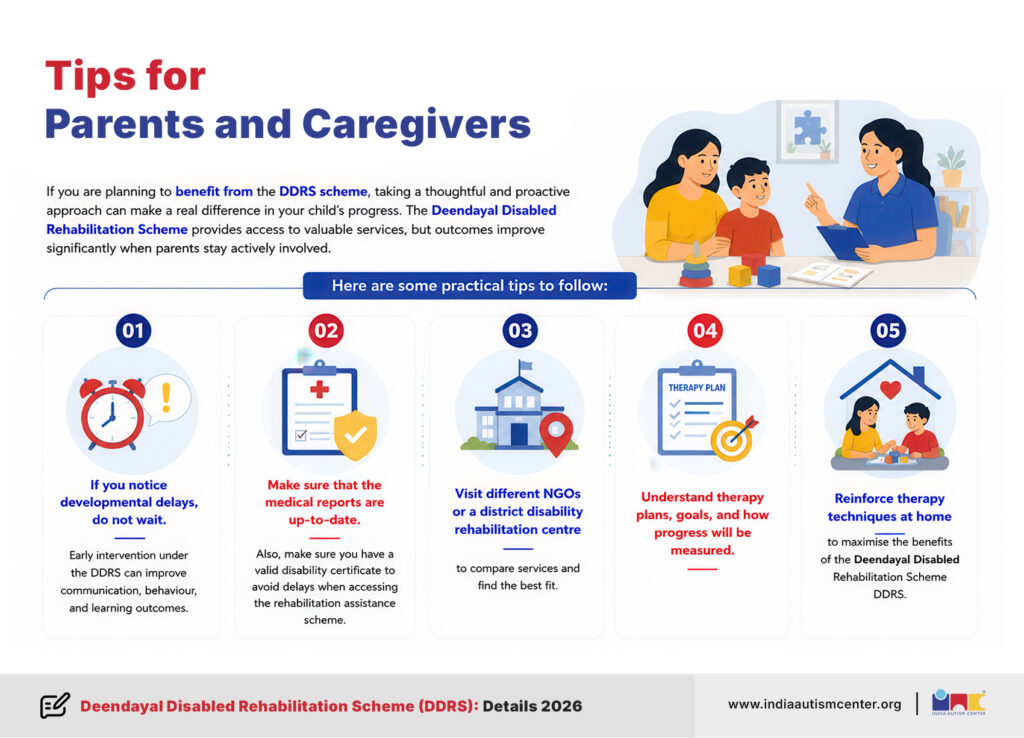
If you are planning to benefit from the DDRS scheme, taking a thoughtful and proactive approach can make a real difference in your child’s progress. The Deendayal Disabled Rehabilitation Scheme provides access to valuable services, but outcomes improve significantly when parents stay actively involved.
Here are some practical tips to follow:
1. If you notice developmental delays, do not wait. Early intervention under the DDRS can improve communication, behaviour, and learning outcomes.
2. Make sure that the medical reports are up-to-date. Also, make sure you have a valid disability certificate to avoid delays when accessing the rehabilitation assistance scheme.
3. Visit different NGOs or a district disability rehabilitation centre to compare services and find the best fit.
4. Understand therapy plans, goals, and how progress will be measured.
5. Reinforce therapy techniques at home to maximise the benefits of the Deendayal Disabled Rehabilitation Scheme DDRS.
Future of DDRS in India

The DDRS has a strong foundation for disability rehabilitation in India. Still, the future is expected to depend on how well it evolves to meet increasing demand, especially in areas like autism and developmental disabilities.
As awareness grows, more families are likely to seek structured support through the DDRS scheme, making it essential to strengthen both reach and quality.
One of the key priorities should be expanding services into underserved regions. Many rural areas still lack access to a fully functional district disability rehabilitation centre, which limits the effectiveness of the rehabilitation assistance scheme.
At the same time, there is a pressing need to train more therapists, special educators, and caregivers to address the shortage of skilled professionals.
Technology can also play a major role. Tele-rehabilitation and digital tools can help extend the benefits of the Deendayal Disabled Rehabilitation Scheme to families who cannot travel frequently.
Additionally, increasing awareness and ensuring faster, more transparent funding will be critical to improving the long-term impact of the Deendayal Disabled Rehabilitation Scheme DDRS.
Conclusion

The Deendayal Disabled Rehabilitation Scheme represents a promise from the government to its most vulnerable citizens. By supporting the DDRS, we are not just funding buildings or salaries; we are investing in the potential of human beings.
Whether it is a child learning to communicate for the first time at a DDRS scheme-funded centre or an adult gaining employment through a rehabilitation assistance scheme, the impact is life-changing.
For every parent reading this, remember that you are not alone in this journey. The Deendayal Disabled Rehabilitation Scheme DDRS and the network of district disability rehabilitation centre facilities are there to support you. By staying informed and utilising these government resources, we can ensure that every individual with a disability has the opportunity to shine.
The path to inclusion is long, but with the right support from schemes like the Deendayal Disabled Rehabilitation Scheme, it becomes a journey of hope and achievement.
Frequently Asked Questions
What is DDRS in simple terms?
The DDRS is a government scheme that funds NGOs to provide rehabilitation services like therapy, education, and skill training for persons with disabilities across India.
Is DDRS only for physical disabilities?
No, the Deendayal Disabled Rehabilitation Scheme covers multiple disabilities, including autism, intellectual disabilities, and sensory impairments.
Are services under DDRS free?
Many services under the Deendayal Disabled Rehabilitation Scheme DDRS are free or highly subsidised, depending on the organisation and type of support provided.
Can adults with autism benefit from DDRS?
Yes, the rehabilitation assistance scheme includes vocational training and life skills programs for adults with autism and other disabilities.
Can NGOs apply for multiple projects under the DDRS scheme?
Yes, eligible NGOs can apply for multiple projects under the DDRS scheme, provided they meet infrastructure, staffing, and compliance requirements set by the government.
How does DDRS support inclusive education?
The Deendayal Disabled Rehabilitation Scheme DDRS supports special schools and resource centres that help children transition into inclusive education environments with proper support systems.
How can DDRS improve long-term outcomes for children with autism?
By providing early intervention, therapy, and skill-building programs, the Deendayal Disabled Rehabilitation Scheme DDRS helps improve independence, communication, and overall quality of life.