Every parent is eager to hear their child’s first words, regardless of whether it is as simple as “no”. But what happens when those words take longer to come? You might start to wonder: Is my child just a late talker, or could it be something more, like autism?
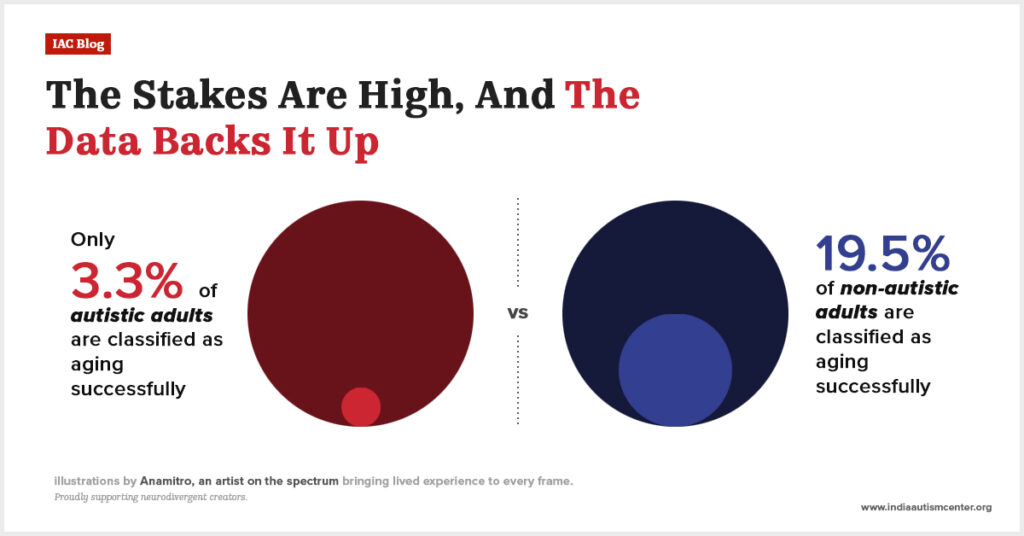
It is a natural question that comes to mind. Especially when speech delay is a common occurrence in children aged 3 to 5 years. On the other hand, globally, about 0.77% of children are diagnosed with ASD (Autism Spectrum Disorder).
Because both conditions can present as “delayed speech”, it’s easy for parents to feel confused or even alarmed when milestones don’t align.
The good news is that speech delay and autism are not the same. Understanding the subtle yet important differences between the two can help you take the right steps early, whether that means seeking speech therapy, undergoing development, or simply requiring more time and support.
Today, we will explore the speech delay vs autism and discuss what parents and caregivers can do to support individuals with these conditions.
Understanding Speech Delay

In simple terms, speech delay is when a child is unable to produce words or sentences in comparison to other children their age. However, the pattern of learning typically follows a similar path.
Children with speech delay typically understand what’s being said to them (their receptive language) but struggle to express themselves verbally (expressive language).
For example, they may follow instructions such as “Bring your shoes,” but they may not be able to say “shoes here” or even “I want shoes.”
Some of the most common speech delay symptoms include:
- Limited babbling by 12 months
- No single meaningful words by 16–18 months
- Not combining words by age 2 (e.g., “want juice”)
- Speech that’s difficult for even the family to understand
- Frequent use of gestures to communicate instead of words
There are different reasons that can lead to speech delay, such as hearing impairment, oral-motor difficulties, cognitive delay, multilingual environments, or simply a “late bloomer” tendency.
In conclusion, speech delay does not imply autism.
Understanding Autism Spectrum Disorder (ASD)

Autism, otherwise known as Autism Spectrum Disorder (ASD), is a neurodevelopmental condition which has an effect on communication, social interaction, and behaviour. It is to be noted that speech delay is one of the symptoms of autism, but many more developmental differences define if a child has autism.
Often, children who have autism develop speech delay. Sometimes, a child with autism might not even have a speech delay. However, even when words appear, they may use them in unusual ways (e.g., repeating phrases or scripting lines from TV shows).
Some of the most common autism symptoms include:
- Reduced eye contact or social engagement
- Limited use of gestures such as pointing towards an object or waving
- Lack of response to name
- Repetitive behaviours (flapping, lining up toys, spinning objects)
- Strong preference for routines or sameness
- Sensitivity to sound, touch, or light
- Speech that’s monotone, robotic, or echolalic (repetition of words or phrases)
Contrary to popular beliefs, autism does not happen due to poor parenting, vaccination, or poor diet. It is essentially a neurological and developmental issue. If diagnosed early, with proper treatment, communication, and social skills can improve considerably.
Speech Delay vs Autism: Key Differences
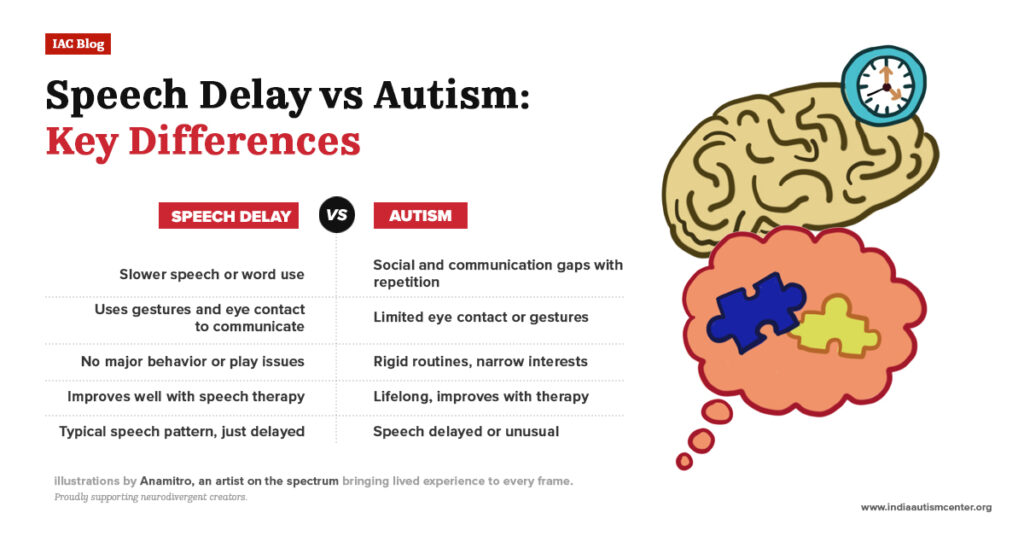
It is a natural phenomenon to feel confused between speech delay as well as autism. However, they are different from one another. When a child struggles with forming or using words, it is a speech delay, while autism involves broader challenges in communication, social interaction, and behaviour.
It is essential to understand the distinction between speech delay and autism, allowing for timely intervention. Here is a side-by-side comparison of speech delay vs autism:
| Feature | Speech Delay | Autism |
| Primary issue | Slower speech development; articulation or word-use lags | Core issues in social communication & interaction + repetitive behaviours; speech may be delayed or atypical |
| Social engagement | The child typically uses gestures, points, makes eye contact, and tries to communicate non-verbally despite delayed speech. | The child may have reduced eye contact, limited pointing or gesturing, less joint attention and may prefer solitary play. |
| Non-speech behaviours | Usually no major behavioural or play issues beyond the speech domain. | Presence of repetitive behaviours, restricted interests, difficulty with change of routine, etc. |
| Outcome & intervention | With speech therapy and support, many children catch up. | Lifelong profile; early intervention helps significantly, but the condition tends to remain on the spectrum. |
| Speech pattern | Typical pattern but slower; errors in production, short phrases. | Speech may be absent/very delayed or present but atypical (echolalia, literal language, unusual prosody). |
For example, when a two-year-old doesn’t speak but points to objects, imitates gestures, and also plays pretend, speech delay may develop. On the other hand, a child who does not point to any object, tends to avoid eye contact, and often fixates on spinning objects has higher chances of being diagnosed with autism.
Is Speech Delay Autism?

Since it is easy to get confused due to similar symptoms of both speech delay and autism, the reality is that speech delay itself is not autism. However, one of the many symptoms of autism is speech delay when it appears along with social as well as behavioural differences.
Many children with speech delays do not have autism and catch up with therapy, but if other developmental red flags appear, further assessment is needed.
So, is speech delay autism? No, a child with speech delay is not autistic, but every child with autism tends to have speech delay.
Signs that Hint at Autism in the Presence of Speech Delay

Speech delay is an early sign of autism. However, it is not necessarily always the case. Hence, it is essential to recognise the additional signs to look for. Here are some “red flag” behaviours:
- If you find that there is limited babbling by 12 months. Or if there is a loss of babbling.
- No single words by 16 months, or loss of previously acquired words.
- Not pointing at objects, not waving or using gestures to display their interest.
- Doesn’t respond to their name by 9-12 months or seems indifferent.
- Limited eye contact or social smiling.
- Often displays repetitive behaviour, mainly including hand-flapping, spinning objects, or even lining up their toys.
- Strong preference for sameness and difficulty with change.
- Unusual speech: echolalia, literal language, or monotone or robotic prosody.
If many of the listed signs begin to appear, it is time to have a complete evaluation done.
Why Does Making the Distinction Matter?

Understanding whether a child has a speech delay or autism is not about labelling them; it is about finding the right approach to obtain help at the right time. Early and accurate identification allows parents, therapists, and educators to tailor interventions that match the child’s specific needs.
When parents and caregivers understand the difference between speech delay and autism, they can take action and offer support that can have a lifelong impact.

Here is why it is necessary to understand the speech delay vs. autism concepts:
Intervention Timing
Children with speech delays can receive speech-language therapy that can lead to significant catch-up. For autism, early multi-modal intervention (speech, occupational therapy, and behavioural therapy) is linked to better outcomes.
Focused Therapy
For speech delay, focused therapy can be provided to address articulation, sentence formulation, and vocabulary. On the other hand, for autism, more focus is on improving social skills, play skills, sensory regulation, and routine management.
Expectations and Support Services
Families of a child who is diagnosed with autism may have the chance to access specialised services, support networks and long-term planning. Appropriate planning can only be done when a parent understands the distinction between speech delay and autism.
Monitoring and Collaboration
If you treat it as a speech delay but miss warning signs of autism, you might miss an earlier chance to intervene more comprehensively.
What Can Parents and Caregivers Do?

Parents and caregivers have to be aware of communication delays, as they can be both confusing and emotionally distressing. The key is not to panic but to take proactive, informed steps.
There are different steps that parents as well as caregivers have to take, such as seeking a professional evaluation, engaging in early intervention programmes, or using supportive communication techniques at home. It can make a significant difference.
The measures that a parent or a caregiver can take include:
1. Tracking Development Milestones
You can utilise speech or language milestones such as babbling by ~9–12 months, single words by ~16 months, and two-word phrases by ~24 months. If your child is not meeting expected milestones, it is essential to consult a paediatrician, a developmental paediatrician, or a speech-language pathologist.
Reaching out to a professional can help you determine if the issue is just related to speech delay or if other broader developmental or behavioural signs imply autism.
2. Engage in Early Intervention Services
Once you have a diagnosis or developmental report, don’t delay intervention. In India, early intervention programs, such as speech therapy, occupational therapy, and behavioural therapy (like ABA).
These therapies help to improve communication, cognitive development, and social interaction skills. The earlier the therapy begins, the more effective it tends to be.
3. Practise Speech and Communication at Home
Parents have to include interactive activities in their child’s speech development to enhance their child’s speech skills. Here are some actions that can help:
- Reading storybooks aloud every single day
- Naming different objects while playing
- Encouraging to repeat simple words
- Singing rhymes or using picture cards
It will strengthen both expressive and receptive language and also create a positive communication environment.
4. Observe and Encourage Social Interaction
Social reciprocity is a common challenge that children with autism face. Some symptoms include difficulty making eye contact, difficulty sharing joy, and not responding to their name when called.
It is essential to foster small but meaningful interactions through play-based learning, where communication occurs naturally and organically. You can encourage children to get engaged in playing turn-based games or engage in pretend play, which helps build joint attention and empathy.
5. Stay Patient and Consistent
Parents/caregivers need to understand that progress will not happen overnight. Whether your child is receiving speech therapy or autism support, consistency and emotional reassurance matter most.
It is important to celebrate even minor milestones. Moreover, a calm environment is to be maintained. It also helps to keep routines predictable, as it provides a sense of safety for children with communication difficulties.
6. Join Support Networks and Communities
Parents who have children with such concerns can feel quite calm yet empowered when they connect to other parents with similar experiences. You’ll gain practical tips, emotional support, and access to professionals who specialise in both speech delay as well as autism management.
How Does Therapy Differ for Speech Delay vs. Autism?

Even though certain symptoms are similar for speech delay and autism, the treatment approaches for speech delay versus autism are quite different. Understanding these distinctions helps parents choose the right kind of intervention tailored to their child’s unique developmental needs.
Here is a side-by-side comparison of how therapy differs for speech delay versus autism:
| Therapy Focus | Speech Delay | Reading aloud, naming objects, and interactive play |
| Main Goal | Improve articulation, vocabulary, and sentence use | Enhance communication, social understanding, and behavioural regulation |
| Approach | Speech-language therapy, parent modeling | Multidisciplinary: speech, occupational, behavioural (ABA) |
| Home Support | Visual schedules, sensory integration, and structured social activities | Visual schedules, sensory integration, structured social activities |
| Expected Outcome | Catching up to peers within 6–12 months of therapy | Gradual progress; lifelong communication growth with continuous support |
When to Seek Professional Help?
Do not wait for the condition to get worse. Once you find the signs below, it is time to seek professional help:
- Isn’t babbling by 12 months
- Doesn’t say single words by 16–18 months
- Doesn’t combine words by 24 months
- Doesn’t respond to their name or show interest in people
- Avoids eye contact or play interaction
You can consult a speech-language pathologist or a developmental paediatrician. If you get early screening for your child, it can help in better identification.
Conclusion

Whether it is speech delay or autism, it can tend to confuse parents and make them concerned, as the symptoms overlap. A speech delay mainly has an effect on a child’s ability to use or understand language, while autism involves broader challenges in communication, behaviour, and social connection. Identifying the distinction will help the child receive the right help.
With actions including early detection, consistent therapy, and compassionate guidance, children with communication challenges can make remarkable progress. Ultimately, it is essential to recognise that each child is unique and develops at their own pace.
Frequently Asked Questions
Is speech delay the same as autism?
No, they are not the same. Speech delay affects a child’s ability to produce or use words, while autism (ASD) involves challenges in social communication, sensory processing, and behaviour. Some children with autism may have speech delays, but not all children with speech delays have autism.
What are the common symptoms of speech delay?
Typical speech delay symptoms include limited vocabulary for age, unclear speech, difficulty forming sentences, and frustration when trying to communicate. However, these children typically show an interest in interacting with and understanding others.
What causes speech delay?
Speech delay can result from hearing loss, oral motor issues, bilingual exposure, lack of stimulation, or neurological conditions. It doesn’t necessarily indicate autism, but it may need professional assessment to identify the cause.
How is autism diagnosed?
To diagnose autism, developmental assessments, observing the child’s behaviour, and standardised tools like the ADOS (Autism Diagnostic Observation Schedule) are used.
For expert insights, support services, and inclusive learning initiatives, visit the India Autism Center.